Rise Of The Superbugs
 When penicillin and other antimicrobials became widely available after World War II, it was not long before their pathogenic targets began developing resistance to the drugs that were meant to quash them.
When penicillin and other antimicrobials became widely available after World War II, it was not long before their pathogenic targets began developing resistance to the drugs that were meant to quash them.
Drugs such as streptomycin, chloramphenicol, tetracycline and sulfonamide have lost much of their original potency, leaving us in a battle against the rise of the multi-drug- resistant “superbugs”.
Supplements which support normal gut immune function reduce pathogenic invasion without the problem of resistance, and can safely be used alongside antimicrobial therapy, or as stand-alone treatment where drug therapy fails or compromises your health.
Infection by drug-resistant pathogens was once confined to the hospital setting, however, the battle lines have now extended beyond the hospital wards, and community-acquired resistant infections are becoming both more commonplace and virulent.
Some of the “superbugs” seen in Australia in both hospital and community settings include:
- Methicillin-resistant Staphylococcus aureus (MRSA)
- Vancomycin-resistant Enterococci (VRE) (e.g. Enterococcus faecalis, E. faecium)
- Clostridium dif cole-associated disease (CDAD)
- Helicobacter pylori (triple and quadruple therapy-resistant strains)
- Streptococcus pneumoniae
- Multi resistant Pseudomonas aeruginosa
- Multi resistant Escherichia coli
- Multi resistant Klebsiella species
- Multi resistant Enterobacter species
Host Defence
A major deficit of modern medicine is a lack of focus on host resistance. Nurturing host resistance involves a healthy diet and adequate rest, as well as healthy gut flora balance, but this is at odds with our modern lifestyle, dietary practices, and reliance on antibiotics which disturb gut flora.
A newer approach of integrative medicine, incorporating drug therapy alongside natural therapies is desperately needed.
Probiotics
Probiotics (“pro”- for, and “bios”- life) offer many health benefits for humans, including synthesis of B vitamins and vitamin K, secretion of antimicrobial substances, and modulation of the immune system, as well as preventing pathogens from occupying spaces along the gastrointestinal tract (GIT).
A non-pathogenic, therapeutic, probiotic yeast called Saccharomyces cerevisiae (boulardii) (SB) has shown efficacy in treating various types of drug-resistant infection and associated diarrhoea.
When used in milligram doses, usually 250mg 3-4 times/day,
SB’s antipathogenic effect is useful in:
- Antibiotic-associated diarrhoea
- Clostridium dif cole-associated diarrhoea (CDAD)
- Irritable bowel syndrome (IBS)
- Helicobacter pylori infection (in adults and children)
- HIV-associated diarrhoea
- Enterotoxic E. coli infection
- Candida albicans infection
- Crohn’s disease
- Diarrhoea in children
- Prevention of diarrhoea during tube feeding (adults and preterm infants)
A significant drawback of probiotic treatment is that its effect may not be immediate.
MedLab SB 5B contains 5 Billion CFU per capsule. This formula is also dairy free.
For immediate relief from antibiotic-associated diarrhoea, CDAD, rotavirus, and other gastrointestinal infections, adjunctive treatment with colostrum is recommended.
Colostrum: Instant Immunity
Colostrum is the breast milk expressed by lactating mothers for their babies. It serves as a ready-made, active immune system to protect the newborn in the first weeks of life when their own immune system is still immature.
One of the rare natural medicines that act extremely quickly, colostrum kills or neutralises a diverse range of pathogens, helps resolve and soothe gut inflammation, and aids in replenishing normal flora in the compromised GIT. Colostrum is rich in immunoglobulins (Ig) including IgG and secretory IgA (sIgA), as well as antimicrobial peptides and growth factors.
There are two types of immunoglobulins present in colostrum: IgG and secretory IgA. IgG protects against a broad range of bacteria, toxins, and viruses in body fluids. Secretory IgA is secreted in saliva, tears, breast milk and mucus secretions, protecting mucous linings in the body (e.g. the intestinal, respiratory and genito-urinary tracts) from pathogens and inflammation.
Bioceuticals GastroCare Excel contains IgG & IgA, lactoferrin and lactoperoxidase.
Lactoferrin and Lactoperoxidase
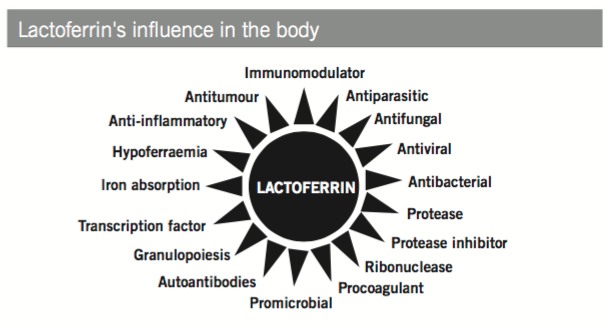
Lactoferrin and lactoperoxidase are antimicrobial peptides contained in colostrum. Their effects on human health have been widely studied. Lactoferrin binds to iron and aids its absorption into the body, at the same time preventing the proliferation of iron-requiring pathogens such as C. albicans.
Lactoperoxidase uses peroxide radicals to damage pathogen cell walls. Neither lactoferrin nor lactoperoxidase from colostrum have damaging effects on normal flora.
In fact, lactoferrin has been reported to have bifidogenic properties.
Safety of Colostrum
Colostrum has been safely consumed throughout history and in many cultures. Today it is used both orally and topically to assist the adherence of probiotics to the gut wall and to decrease in ammation in in ammatory gut diseases, thrush, nappy rash and some fungal skin infections.
Even in severely immune-compromised patients, colostrum has been safely used to treat CDAD and infectious diarrhoea.
There is low incidence of intolerance problems with the use of colostrum and clinically relevant side effects are limited to possible sensitivity to milk proteins and intolerance to lactose.
However, in lactose intolerant individuals, colostrum products containing 0.4 grams of lactose per 5g dose (1 heaped teaspoon) can be tolerated in quantities of approximately 15 teaspoons per day by even the most sensitive of sufferers.
Final Word:
As we struggle to stay ahead of the “superbugs” with newer and stronger antibiotics, a focus on host resistance may nally give us an unbeatable advantage. Products such as colostrum which contain lactoferrin and lactoperoxidase, as well as high levels of the immunoglobulin fractions secretory IgA and IgG, show promise in supporting host resistance.
They can be mixed with probiotics of all types, including all species of lactobacilli, bifidobacteria and SB, and taken alongside any antimicrobial, antidiarrhoeal or antispasmodic medication, to enhance current strategies against drug-resistant infections.
Further Reading: